
Findings from the Comprehensive Care for Joint Replacement (CJR) third annual evaluation 报告 demonstrate that bundled payments for lower-extremity joint replacements (LEJR) reduce Medicare expenditures. 在前三年的业绩中, 法定医院:
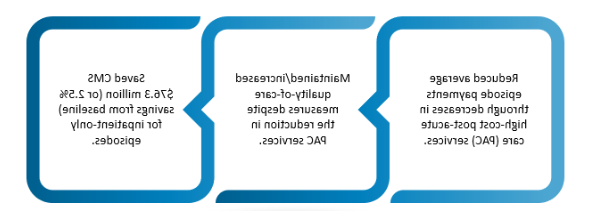
然而, the 2018 rule change allowing LEJRs in the outpatient setting may impact the model’s ability to achieve savings in later performance years. To address these declining savings, CMS issued a 拟议的规则 in early 2020 that would incorporate outpatient hip and knee replacements into the episode of care definition and extend the model another three years. Commercial payers have also introduced policies that transition cases to the outpatient setting.
鉴于这种预期的市场转变, providers should take note of the following key findings to ensure their orthopedic service line is designed for future success, regardless of their participation in the CJR model.
更大的容量带来更高的节省
根据评估报告, “the average reconciliation payment per episode was higher for hospitals that had higher composite quality scores, LEJR体积更高, 我们不是为了盈利, and served less-complex patient populations.[1] Lower-volume hospitals typically aren’t able to realize the efficiency gains from economies of scale or care standardization that higher-volume facilities can, and the impact of repayments to CMS can be significant—particularly as target prices decrease. Now may be the time to consider rationalizing LEJR cases at low-volume facilities and performing them at a single, high-volume location within your health system.
内部改进是不够的
在第三个演出年度, a lower proportion of CJR participant hospitals earned reconciliation payments than in previous years, since a larger share of the target price was based on the regional average episode payments.[2] Focusing on internal savings may create gainsharing opportunities with your surgeons, but it won’t generate reconciliation payments at the end of the performance year. And with the potential inclusion of outpatient cases beginning in 2021, 混合目标价格可能会下降. Continuing to focus on reducing the total episode cost will be critical for generating ongoing reconciliation payments.
合作是成功的关键
The relationships between the hospital and orthopedic surgeons shaped hospitals’ responses to the CJR model.[3] 医院 that employed their surgeons often had success collaborating on the development and implementation of care redesign initiatives, whereas hospitals that did not employ their surgeons ran into barriers (e.g., physician ownership of competing ambulatory surgery centers).
For those hospitals that do not employ their physicians, developing an effective physician alignment strategy, 比如管理, or implementing a CJR gainsharing program will encourage collaboration on cost-saving efforts, enhance physician support for quality and process improvement initiatives, and promote patient-centered care redesign efforts.
The shift to outpatient settings is inevitable
评估发现,总的来说, “法定医院 were less likely than other hospitals to provide TKA in the hospital outpatient setting.[4] 然而, participants that transitioned a higher of volume of cases to the outpatient setting 报告ed numerous keys to their success, such as “establishing an outpatient default status for all TKA patients, enhancing internal documentation review and auditing processes, 修改或创造新的算法, 进气形式, 或者其他工具.[5]
With the proposed inclusion of lower-cost outpatient cases in the episode of care definition, target prices will likely experience an immediate and potentially significant decrease. Those hospitals that continue to perform knee and hip replacements in the inpatient setting may struggle to generate enough savings to receive reconciliation payments from CMS. 而不是等待这一切发生, service line leaders should begin to act on these findings now in order to be prepared for the policy change.
展望未来
CMS is committed to testing a mandatory bundled payment model that relies on regional spending benchmarks, regardless of where the surgery takes place. 鉴于这种演变, providers should consider proactive strategies that put them in a position to manage the near-team landscape, which will include shifts in volume and risk arrangements.
Would you like to develop a modern orthopedics program?
Learn how to build a destination center for patients. 阅读我们的文章, 开发一个 现代骨科目的地计划.
阅读文章脚注
- 1.
从110页发现, 第三次年度报告,CJR评估- TOC
- 2.
从109页发现, 第三次年度报告,CJR评估- TOC
- 3.
从114页发现, 第三次年度报告,CJR评估- TOC
- 4.
CJR participant hospitals have financial incentive to perform TKAs in the inpatient setting. If CJR participating hospitals move less costly patients to the outpatient setting, the remaining inpatient population would be costlier than the historical population used to calculate target prices and would make it harder for hospitals to reduce their payments below their target price and thus lower reconciliation payments
- 5.
从121页发现, 第三次年度报告,CJR评估- TOC
2021年2月10日发布